Key takeaways
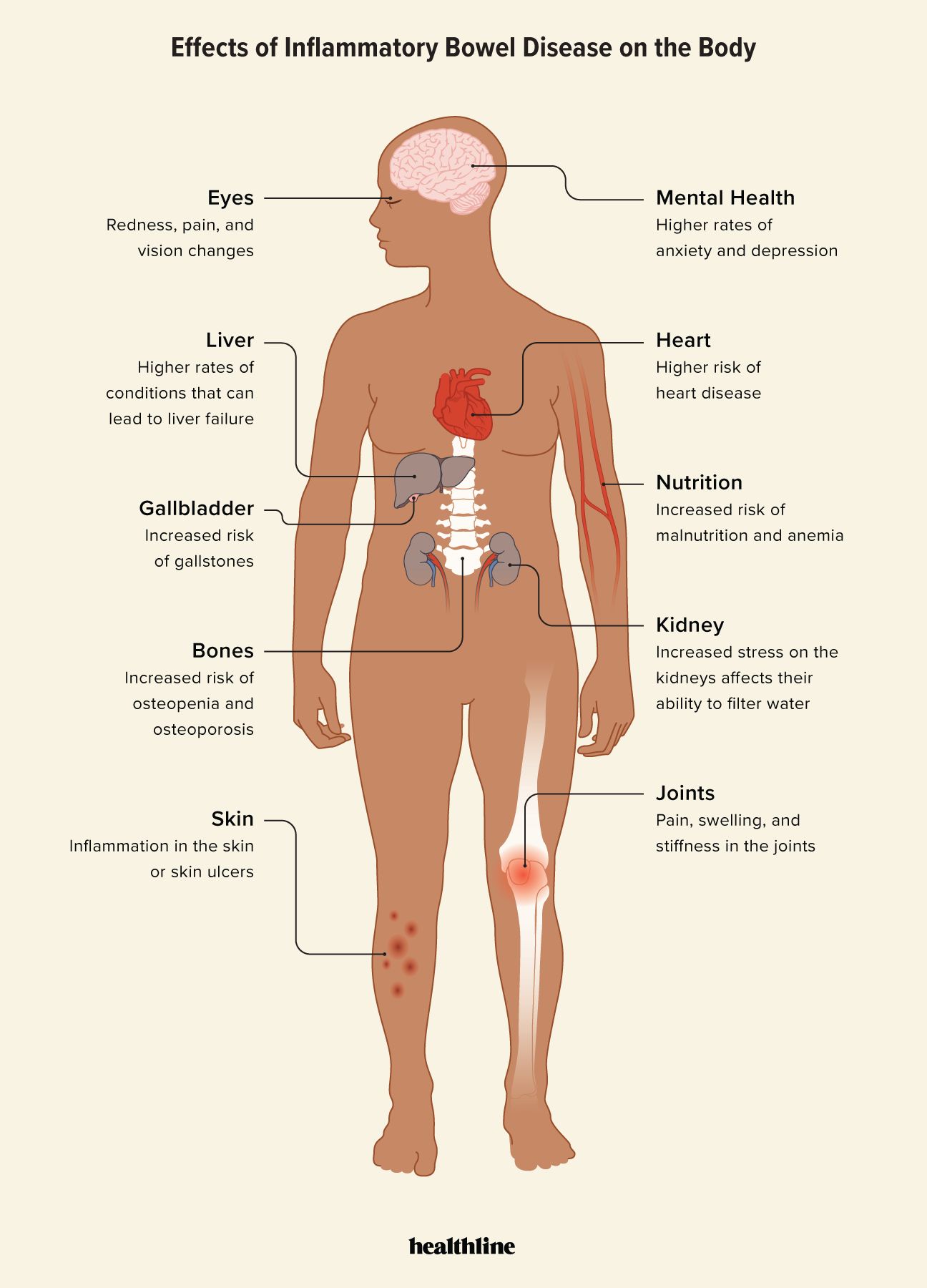
- The effects of inflammatory bowel disease (IBD) can extend beyond the digestive system, affecting various parts of the body due to ongoing inflammation.
- IBD can lead to potential complications such as reduced bone density, joint pain, nutritional deficiencies, and issues with your liver, gallbladder, kidneys, and heart.
- Monitoring for changes in your physical and mental health and maintaining open communication with your care team are key to managing the full-body effects of IBD.
Inflammatory bowel disease (IBD) is often thought of it as a disease of the digestive tract. While digestive symptoms are a defining feature of a flare, the effects of IBD can extend well beyond the gut.
Ongoing inflammation is the main driver of these effects. Inflammatory proteins released by the immune system can travel beyond the digestive system and affect otherwise healthy tissue, leading to a range of complications. Changes in your diet or gut bacteria may also play a role. In some cases, medications used to manage IBD can increase the risk of additional health conditions.
Learn how IBD can affect other areas of your body, what signs to watch for, and steps you can take to support your overall health.
Bones are made of living tissue that constantly breaks down and rebuilds to stay strong. When bone loss happens faster than bone formation, bones become weaker and more prone to fractures.
Up to 70% of people with IBD have bone density below the normal range. This is known as osteopenia. Osteoporosis is a more severe form of bone loss, where bones become increasingly fragile.
Chronic inflammation from IBD can directly affect bone tissue and increase mineral loss. Long-term use of corticosteroid medications, which are sometimes used to control IBD flares, can further accelerate bone loss.
Nutrition also plays a key role in bone health. If IBD symptoms make it difficult to eat enough, or if inflammation in your digestive tract interferes with nutrient absorption, it can be hard to meet your recommended intake of key nutrients that support bone health, including:
- calcium
- vitamin D
- vitamin K
- magnesium
Because osteopenia and osteoporosis often don’t cause any noticeable symptoms, it’s important to talk to your doctor about bone mineral density testing and how often you should be screened.
About 50% of people with IBD experience joint pain, swelling, or stiffness. When these symptoms occur without inflammation, it’s called arthralgia.
When inflammation is present, it can indicate a type of arthritis associated with IBD called peripheral arthritis. There are two main forms:
- Type 1 peripheral arthritis: This is the most common type of arthritis in IBD. It affects
larger joints in the arms, legs, hands, and feet. It tends to flare up alongside IBD symptoms. Treatments for IBD often help ease type 1 peripheral arthritis, as well. - Type 2 peripheral arthritis: This targets smaller joints, and is not linked to IBD flares. In fact, in some cases, it develops
before an IBD diagnosis. This type requires its own treatment outside of IBD, which may include medication or physiotherapy.
Talk to your care team if you notice any changes in your joints.
Good nutrition is important for everyone, but it’s especially crucial when you have IBD. Malnutrition and low nutrient levels, including iron deficiency anemia, are common in IBD.
IBD symptoms like pain, fatigue, low appetite, and ongoing digestive issues can make it difficult to eat enough. Worries about certain foods triggering your symptoms may also limit what you feel comfortable and safe eating. In addition, inflammation in the digestive tract can reduce nutrient absorption.
Anemia can develop if you’re not getting enough iron or other nutrients. Blood loss during an IBD flare further increases your risk of anemia.
There are steps you can take to improve your nutrient status. Ask to your care team about checking your nutrient levels and discuss whether vitamin or mineral supplement may be needed.
If you’re having trouble eating enough, talk to a registered dietitian who specializes in IBD to help you develop a safe, balanced eating plan.
Your liver and gallbladder work together to support digestion. The liver produces bile, the gallbladder stores it, and a network of ducts carry bile to where it’s needed throughout the body.
Changes in your liver and gallbladder health are among the most common extraintestinal manifestations of IBD. Up to 30% of people with IBD have abnormal liver function test results, and around 5% may develop liver disease. Inflammation in the liver, gallbladder, or bile ducts, along with changes in the gut microbiome, can contribute to:
- Primary sclerosing cholangitis (PSC): PSC occurs when the bile ducts become inflamed and narrow. This blocks the normal flow of bile and can potentially lead to liver failure. PSC is closely linked to IBD, as up to 70% of people with PSC also have IBD.
- Autoimmune hepatitis: This is another inflammatory liver condition that can progress to liver failure. It’s rare, but more common in people with IBD compared to the general population.
- Gallstones: People with IBD are more likely to develop gallstones compared to the general population. These are deposits that build up in your gallbladder and may block a duct, leading to severe pain.
Regular blood tests can help monitor liver enzyme levels and catch changes early. Talk to your care team about how often you should be screened.
Your kidneys filter your blood, removing waste and excess fluid. When kidney function is impaired, waste products can build up in your blood. IBD can affect your kidney health in a few ways.
During a flare, fluid loss and dehydration put stress on your kidneys. Malnutrition and ongoing inflammation in your body are also hard on your kidneys. Additionally, some medications used for IBD can damage your kidneys.
The two most common kidney conditions seen with IBD include:
- IgA nephropathy: This develops when excess antibodies build up in the tiny filters in the kidneys, causing damage.
- Interstitial nephritis: This happens when the spaces between the small tubes in the kidneys becomes inflamed, which can be acute (short-term) or chronic (long-term)
To monitor kidney health, your care team may recommend regular blood and urine tests to track kidney function.
Inflammatory conditions like IBD can increase the risk of heart disease. Increased levels of inflammatory proteins during a flare of IBD can damage blood vessels, contributing to heart issues.
Some research suggests that people with IBD may develop heart disease at a younger age compared to those without IBD.
Heart disease is influenced by both controllable and uncontrollable risk factors. While you can’t change some risk factors, there are steps you can take to protect your heart, including:
- eating a healthy diet
- staying active
- finding ways to lower stress
- managing IBD to reduce inflammation in the body
Talk with your care team about how often to check your blood pressure, blood sugar, and cholesterol levels. If needed, take medication as directed to help manage these risks.
In some cases, IBD can affect the skin. Two of the most common skin conditions seen in people with IBD, though still rare, include:
- Erythema nodosum: This occurs when the fat under your skin becomes inflamed. It causes reddish-purple lumps, usually on the shins. These lumps
often appear during an IBD flare and tend to improve during remission. - Pyoderma gangrenosum: This is a skin condition that causes painful skin ulcers that develop quickly. Like erythema nodosum, these ulcers often improve with effective IBD treatment.
It’s important to monitor your skin for any changes, especially during an IBD flare, and report any new or worsening symptoms to your care team
IBD can sometimes affect the eyes. Certain inflammatory eye condtions are common in people with IBD, including:
- Episcleritis: This causes redness and irritation in the clear layer covering the white of your eye, though often improves as digestive symptoms get better. While episcleritis is a more common IBD-related eye complication, it’s not usually serious.
- Scleritis: This affects the white of your eye. Scleritis can cause more severe pain and changes in your vision. Surprisingly, it’s more likely to appear when IBD is in remission.
- Uveitis: This affects in the uvea, the middle layer of your eye. Research suggests that changes in the gut microbiome may help explain the link between IBD and uveitis. Early treatment is essential to prevent vision loss.
Watch for any changes in your eyes, including redness, pain, light sensitivity, or vision changes, and report any new symptoms to your care team.
The effects of IBD can extend beyond your body and impact your mental health. People with IBD have higher rates of anxiety and depression compared to those without the condition. Several factors contribute to this risk, including the unpredictability of symptoms like chronic pain and fatigue, as well as isolation due to symptoms.
Ongoing research is exploring the gut-brain axis, which looks at how your brain and gut health influence each other.
Please talk to a loved one or your care team if you’re worried about your mental health. You don’t have to manage this alone.
While IBD is often thought of as a disease of the digestive tract, it can affect many parts of the body. Some related conditions flare up alongside digestive symptoms, while others appear even when IBD seems well-controlled.
Because of these wide-ranging effects, it’s important to have a full healthcare team supporting you. Regular bloodwork can help monitor your nutrient levels, liver health, kidney function, and heart health. Your care team may recommended other tests as-needed.
Pay attention to any changes you notice in your body or mental health, and share them with your care team. Early communication and monitoring can help you stay as healthy as possible.